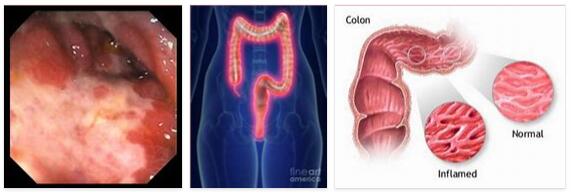
Important functions of the human organism are ascribed to the large intestine with digestion and immune defense. It is therefore all the more problematic if inflammation develops in the colon. Because colon inflammation is characterized in acute phases by serious symptoms, which can lead to life-threatening complications if treatment is not taken.
What is Colon Inflammation?
Colonitis is a chronic inflammatory disease of the large and rectum, which is also known as ulcerative colitis in medical jargon. According to abbreviationfinder.org, the inflammation only affects the uppermost layer of the intestinal mucosa, in which bleeding ulcers can develop.
In addition, those affected by colon inflammation are also affected by the rectum, from which the disease can spread in various directions. A complete cure of the inflammation of the large intestine has not yet been possible, but the symptoms can be narrowed down as far as possible using appropriate treatment methods. Colonitis is often confused with Crohn’s disease.
However, this disease only affects the small intestine, in which several layers of the skin become inflamed. Inflammation of the large intestine usually affects males between the ages of 16 and 25, although only in Germany about 20 people per 100,000 inhabitants fall ill every year.
Causes
The exact causes of colon inflammation have not yet been clarified exactly. However, it is believed that the inflammation is caused by the patient’s genetic makeup. In this way, special genes were discovered which exist in a different form in the body when colon inflammation is present.
In addition to hereditary components, certain risk factors can also increase the likelihood of an illness. On the one hand, this includes nutrition, as certain foods with a high proportion of lactose are often not tolerated by the patient. On the other hand, a malfunction of the immune system can promote inflammation of the large intestine.
Even after surgical removal of the appendix or after giving up tobacco there is an increased risk of the disease. Psychosomatic reasons, on the other hand, are excluded as the cause of colon inflammation.
Symptoms, ailments & signs
Depending on the individual course of the disease, colon inflammation can have a different appearance with varying degrees of severity of the symptoms. In general, inflammation of the large intestine is only insidious at first and only shows severe symptoms in later stages. Sometimes the disease occurs suddenly without any prior signs.
During an acute phase of the illness, severe diarrhea is the defining characteristic of colon inflammation. This diarrhea can occur up to forty times a day and often has bloody and slimy secretions. The bowel movement is generally very painful and can often result in fecal incontinence, in which those affected can no longer control their stool.
Patients with colon inflammation also show flatulence, which is usually caused by a sugar intolerance. The symptoms described are also accompanied by strong, wavy abdominal pain in the lower abdomen, which is referred to as colic in medical terminology. Colic occurs as a result of spasmodic muscle contractions in the muscles of the large intestine and can cause nausea and vomiting in the patient.
Furthermore, a considerable acceleration of the heartbeat to 100 beats per minute is possible, which in extreme cases can lead to circulatory collapse. In general, acute flare-ups also lead to a general deterioration in the state of health, in that performance, energy and weight decrease. In more rare cases, attacks of fever and inflammation of the joints, skin or eyes also occur.
Diagnosis
The diagnosis of colon inflammation is divided into two basic parts. First of all, the patient’s individual medical history is recorded as part of an anamnesis, before a physical examination is carried out in the next step. This examination is usually a colonoscopy, during which an examination instrument, the so-called endoscope, is inserted through the anus.
The condition of the mucous membranes and possible inflammation can then be assessed. Also pus deposits can be detected by this methodology. Furthermore, it is possible to take tissue samples, which are used for microscopic examination in the laboratory and thus provide an exact result. If there is a hardened suspicion of colon inflammation, a second reflection is carried out at a later point in time to confirm the diagnosis.
The interval between colonoscopies depends on the patient’s state of health. In addition to a colonoscopy, if colon inflammation is suspected, a blood count is also taken. In particular, the hemoglobin value and the value of the so-called C-reactive protein are decisive in determining inflammation.
A progressive measurement of the hemoglobin value enables the respective extent of the inflammation and the amount of blood loss to be determined. To further ensure the diagnosis, the liver values can also be determined, which are usually increased by two enzyme values in the case of colon inflammation. The stool is also examined in the laboratory to rule out bacterial infection as the cause of the colon inflammation.
Complications
The conventional symptoms of inflammation of the large intestine can in certain cases be made more difficult by the development of complications. Among other things, it is possible for heavy bleeding to occur during acute relapsing phases, which necessitates inpatient monitoring of the patient.
In affected individuals may be due to bloody diarrhea also an anemia, short anemia develop. A dangerous enlargement of the large intestine, known in medicine as megacolon, is also conceivable. The megacolon is caused by paralysis of the intestine. This in turn results from a steady accumulation of the stool in the intestine, as this no longer moves as a result of the inflammation and cannot transport the stool.
As a further consequence, the intestine can painfully expand in this context, which in turn can pose life-threatening threats such as inflammation of the peritoneum or a rupture of the intestine.
When should you go to the doctor?
When the first signs appear and you feel unwell in the intestinal region, a visit to a doctor is always advisable to clarify the cause of the symptoms. However, a visit from an expert is essential at the latest after symptoms such as bloody diarrhea or severe abdominal pain have occurred. This is particularly useful against the background of possible complications that can occur if the diagnosis or treatment is too late. If possible, a gastrointestinal specialist such as an internist, proctologist or gastroenterologist should be consulted and examined.
Treatment & Therapy
Due to the insufficient clarification of the cause of colon inflammation, existing treatment approaches can only contain the symptoms of the disease. Even if there is no complete cure of the disease, those affected are able to live a completely normal everyday life in symptom-free phases of life.
Maintaining a liquid-intensive, low-fiber, high-calorie diet can have a positive effect on the course of the disease. If the person concerned has lactose intolerance, lactose-free milk products can be used. If, on the other hand, fat absorption is affected, products with so-called MCT fats from diet products should predominantly be consumed.
In this context, anti-inflammatory drugs are often used, which enormously increase the time between two attacks. For drug treatment, 5-ASA preparations are possible, the effect of which is supported by the administration of cortisone if necessary. So-called immunosuppressants can also be taken to suppress the immune system. On the other hand, antibiotics are rarely prescribed.
The respective drugs are usually applied at the point of inflammation where the extent of the inflammation is greatest and the risks are lowest. In special cases, the drugs can also be injected through the bloodstream. Significant deficiency symptoms as a result of severe diarrhea can be combated with vitamin and mineral supplements if a simple change in diet was unsuccessful.
If the course of the disease is particularly severe or is accompanied by complications, surgery is usually essential. During the operation, the large intestine is removed and the small intestine is repurposed so that the affected person can perform a conventional defecation. In some extreme situations, however, the creation of an artificial anus can no longer be avoided.
Outlook & forecast
In the presence of colon inflammation, no clear prognosis can be made. In general, however, it can be said that a complete cure of the disease is still impossible. However, if the inflammation remains limited to the end of the colon and the rectum, a positive course with an average life expectancy can be assumed.
The measure of administering 5-ASA preparations alone reduces the risk of cancer by an enormous 75%. Nevertheless, patients with colitis a significantly increased risk of having a cancer tumor to be formed. On the other hand, if complications of inflammation, such as cancer, occur, life expectancy is considerably reduced if these are diagnosed and treated relatively late. With the help of early surgical or drug treatment, patients can usually live a normal everyday life.
Prevention
Targeted prevention of colon inflammation is not possible due to the uncertain causes of the disease. However, following certain measures can lengthen the quiet phases of the disease, or remission phases, and thereby make everyday life easier for those affected. A generally healthy lifestyle, which is primarily characterized by a balanced diet, is important for this.
So mainly easily digestible foods should be consumed, which are characterized by an optimal nutrient composition. Getting enough exercise is also critical to a healthy lifestyle. Psychological burdens such as stress should also be prevented as much as possible. Due to the increased risk of colon cancer, those affected should have regular check-ups.
Aftercare
In the case of colon inflammation, the person affected usually has only a few measures and options for follow-up care available. The affected person is primarily dependent on the correct and above all on the early treatment of the colon inflammation so that it does not spread to the other organs. If the disease is not treated, it can, in the worst case, lead to death.
Therefore, early diagnosis is the main focus of this disease. In most cases, the disease can be treated with medication, primarily antibiotics. Treatment lasts for about a week, with proper and regular use of the medication. In many cases, after the symptoms have subsided, further follow-up examinations are advisable in order to identify further complaints at an early stage.
The affected person should only eat sparing food during the treatment and only get the stomach and intestines used to the usual food again after the treatment. In many cases, tests should also be carried out for intolerance and allergies that may have triggered the colon inflammation. This can prevent colon inflammation from occurring again.
You can do that yourself
If there is already colon inflammation, those affected can independently reduce the symptoms in addition to the treatment method they have chosen. Sick people are particularly advised to change their diet, known as the avoidance diet. As part of this diet, foods that promote inflammation should be removed from the menu and replaced with anti-inflammatory products. This enables the risk of complications to be reduced and certain symptoms to be alleviated.
Especially during recovery phases, the focus should be on a balanced diet rich in fiber. On the other hand, foods such as milk, oats or cereals can often trigger food intolerances. If there is again a relapse phase, a low-fiber diet is of central importance. Ultimately, however, even following an avoidance diet does not completely cure colon inflammation.